You’ve had the pain before. It eased up. Now it’s back — shooting down your leg, making every step a negotiation. Here’s what’s really happening, and what you can do about it.
🕐 10 min read 📍 Serving Casula, Liverpool, Moorebank, Prestons, Glenfield 📅 Updated April 2025
What Is Sciatica? (And What It Isn’t)
Sciatica isn’t actually a diagnosis — it’s a symptom. When the sciatic nerve, the longest and widest nerve in the human body, becomes compressed or irritated anywhere along its pathway, the result is pain, tingling, numbness, or weakness that radiates from the lower back down through the buttock and into the leg, sometimes all the way to the foot.
The term “sciatica” gets used loosely, which is part of why so many people struggle to get effective treatment. Your GP might diagnose it. The internet offers seventeen different causes. Your neighbour swears by their stretching routine. But without identifying your specific cause, treatment remains a guessing game — and pain keeps returning.
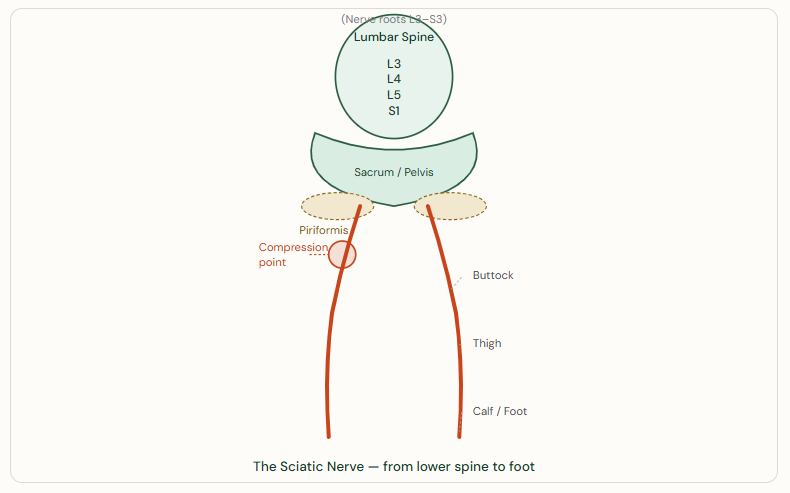
The sciatic nerve originates from nerve roots L3–S3 in the lumbar spine and travels through the buttock, down the back of the leg to the foot. Compression at any point along this pathway causes sciatica symptoms.
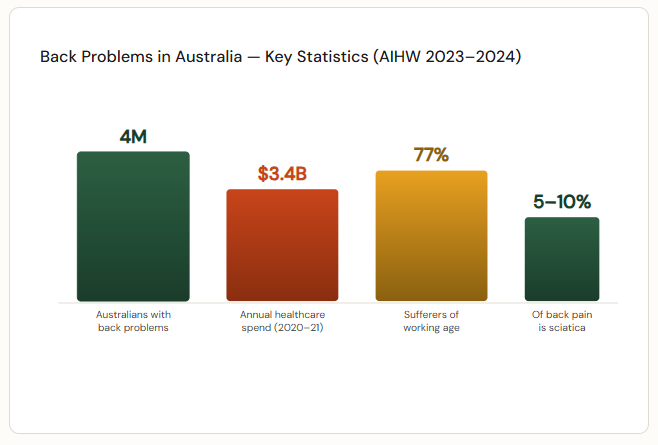
| “Around 5–10% of patients suffering from back pain have sciatica. Back problems were Australia’s third leading cause of disease burden in 2023, affecting approximately 4 million Australians.” Source: Australian Institute of Health and Welfare (AIHW), 2024 |
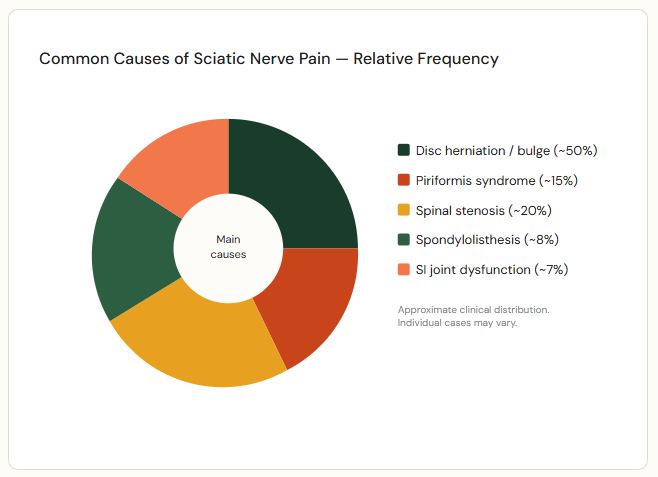
The Root Causes of Sciatica
Sciatica doesn’t just happen. It’s the result of the sciatic nerve being compressed, pinched, or inflamed at one or more points. Understanding your specific cause is the single most important step in fixing it — and in stopping it from coming back.
1. Herniated or Bulging Disc (Most Common)
The discs between your vertebrae act as shock absorbers. When the soft inner material of a disc pushes out through the outer layer, it can press directly on the nerve roots that form the sciatic nerve. This is responsible for the majority of sciatica cases and is commonly triggered by lifting with poor technique, long periods of sitting, or cumulative wear and tear.
2. Piriformis Syndrome
The piriformis is a small muscle deep in the buttock. In some people, the sciatic nerve passes directly through this muscle rather than beneath it. When the piriformis becomes tight or inflamed — from prolonged sitting, hip weakness, or overuse — it squeezes the nerve. This type of sciatica often responds extremely well to dry needling and targeted soft tissue work.
3. Spinal Stenosis
Stenosis is the narrowing of the spinal canal, usually from age-related degeneration, bone spurs, or thickened ligaments. The resulting reduction in space puts pressure on the nerve roots. This type is more common in patients over 50 and tends to cause symptoms in both legs, particularly when walking.
4. Spondylolisthesis
When one vertebra slips forward over another — often at L4–L5 — it can compress the nerve root. This may be caused by a stress fracture (common in athletes) or by degeneration of the facet joints over time.
5. Sacroiliac Joint Dysfunction
The sacroiliac (SI) joint connects your spine to your pelvis. Dysfunction here can mimic sciatica, producing buttock and leg pain through nerve irritation and muscle referral patterns. This is frequently missed in standard GP assessments.
Do You Have Sciatica? The Symptom Checklist
Sciatica has a recognisable pattern, but it varies widely between individuals. Some feel a sharp, electric shock-like pain; others describe it as deep aching, burning, or numbness. Use this checklist to assess your symptoms:

| ⚠ Seek urgent medical attention if you experience: Loss of bladder or bowel control alongside back and leg pain — this may indicate Cauda Equina Syndrome, a rare but serious spinal emergency requiring immediate care. |
Why Does Sciatica Keep Coming Back?
This is the question most patients come to us with. They’ve had relief before — maybe from painkillers, a course of physio, or just waiting it out. But the pain always returns, often worse than before. There are four main reasons this happens.
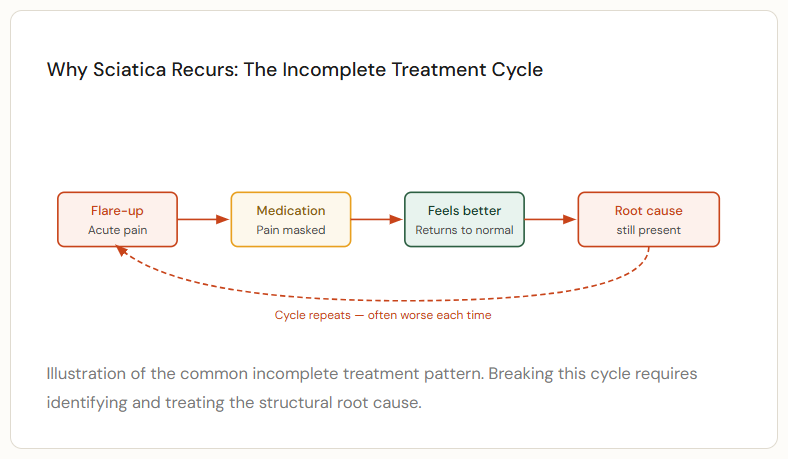
Reason 1: The Root Cause Was Never Addressed
Anti-inflammatory medication and rest reduce inflammation and pain — but they don’t fix a bulging disc, a tight piriformis, or a misaligned vertebra. As soon as you return to normal activity, the mechanical problem reasserts itself and the nerve becomes irritated again.
Reason 2: Contributing Factors Are Still Present
Weak core muscles, poor posture, an inflexible hip flexor, or a sedentary lifestyle all place ongoing mechanical stress on the lumbar spine and sciatic pathway. Without addressing these, any improvement in the clinic will gradually be undone by daily life.
Reason 3: You Were Told to Rest Too Much
Bed rest was once prescribed for sciatica. We now know this is counterproductive. Controlled, specific movement — guided by a practitioner — is far more effective than rest. Immobility allows muscles to weaken and joints to stiffen, making the next episode more likely.
Reason 4: You’ve Only Treated One Part of the Problem
Effective sciatica treatment needs to address the nerve itself, the structure compressing it, the muscles around it, and the movement patterns that allowed the problem to develop. A single-modality approach — medication only, or massage only — rarely achieves this.
What Actually Works: Treatment Options in Casula & Liverpool
At Flame Tree Chiropractic in Casula, we take a multi-modal approach to sciatica — because sciatica is a multi-dimensional problem. Rather than applying a standard protocol, we assess the specific cause of your nerve irritation, then combine treatments to address every layer of the problem.
Here is what the evidence tells us about each treatment approach available at our clinic:


| “A 2024 meta-analysis of over 5,000 patients showed 88% of individuals with acute sciatica achieved significant pain reduction through chiropractic care within 12 weeks of treatment.” Source: Trager RJ et al., PLoS One, 2025 |
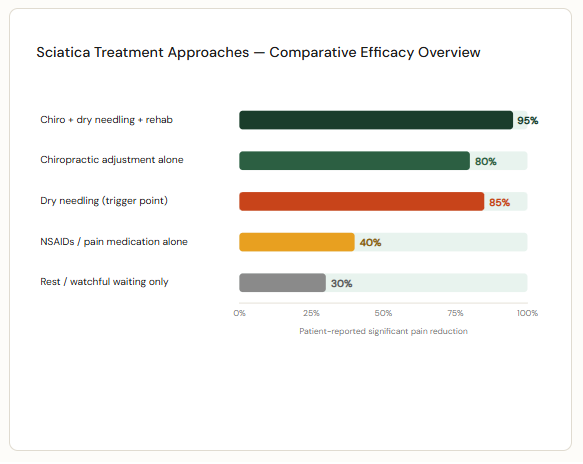
| Compiled from: Trager et al. 2025; Kings Chiropractic Clinical Data 2024; clinical outcome literature review. Figures represent approximate patient-reported outcomes across studies. |
| About Chiropractic & Opioid Risk A 2025 study published in PLoS One found that patients who received chiropractic spinal manipulation for sciatica had a significantly reduced risk of opioid-related adverse events compared to those who did not receive chiropractic care — highlighting the value of non-pharmacological treatment as a first-line option. (Trager et al., PLoS One, 2025) |
3 Safe Exercises for Sciatica Relief (Do These at Home)
These exercises are designed to complement professional treatment — not replace it. If any exercise increases your pain, stop immediately and consult your chiropractor before continuing.

These exercises address the most common muscular contributors to sciatica. Always check with your chiropractor which are appropriate for your specific cause.
What to Avoid When You Have Sciatica
- Prolonged sitting — increases disc pressure by up to 40% compared to standing
- Bending and twisting together — the most common disc-injury movement
- High-impact exercise (running, jumping) during an acute flare
- Self-manipulation — attempting to “crack” your own back can worsen disc problems
Sleeping on your stomach — increases lumbar extension and can aggravate nerve compression

Recent Comments